State bills would remove physician oversight from nurse anesthetists in Stanislaus County
Assemblyman Heath Flora, R-Ripon, has introduced two bills to upgrade the status of nurse anesthetists amid a shortage of physician anesthesiologists in California and controversy in Modesto about hospital policies.
Assembly Bill 876 would give certified registered nurse anesthetists (CRNAs) the long-sought-after authority to practice independently.
If approved and signed into law, the legislation would bring changes for patients in Stanislaus County and the rest of the San Joaquin Valley, where the shortage of physician anesthesiologists is more acute and smaller hospitals struggle to pay their fees.
In the operating room, the person putting the patient to sleep for surgery might not be an anesthesiologist with medical school education and years of residency training. Already at Doctors Medical Center and the Kaiser Permanente hospital in Modesto, a CRNA with supervision from a physician anesthesiologist will likely be involved with a patient’s surgical care.
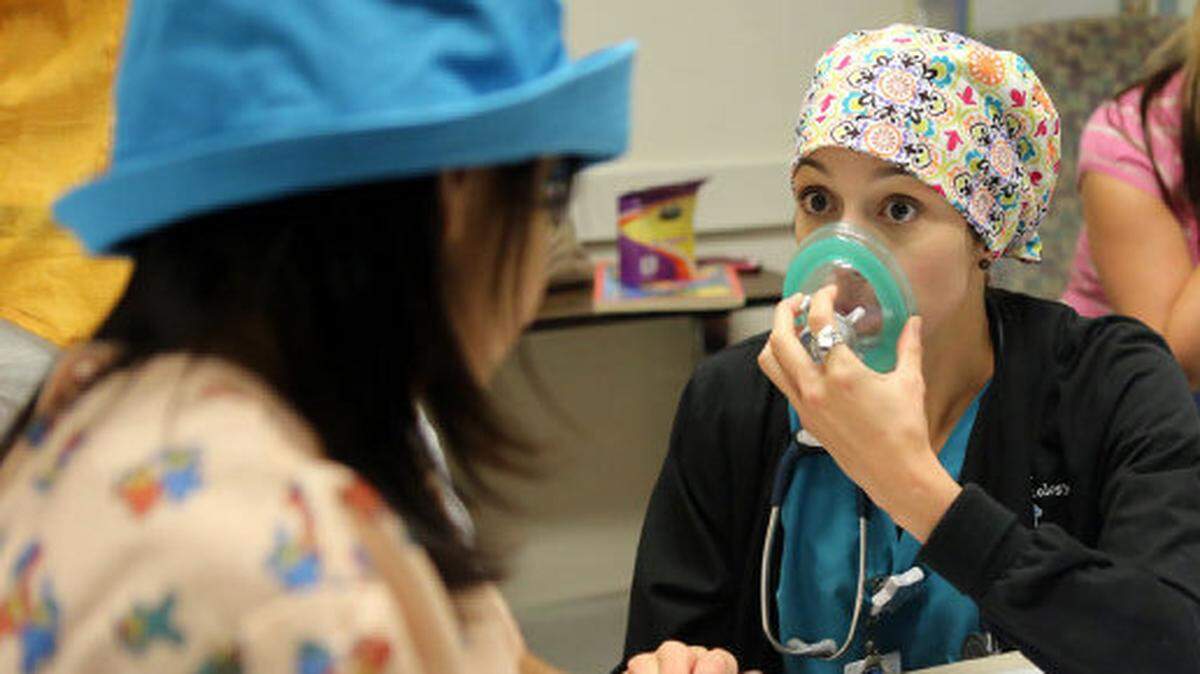
CRNAs, who are critical care nurses with two years of specialized anesthesia training, administer anesthesia and monitor patients during and after surgery. Effective in 2025, new CRNAs must have a three-year doctorate degree.
AB 876 includes a provision that nurse anesthetists would not be limited to the scope of practice of registered nurses in performing anesthesia services. They also would not have to perform anesthesia services pursuant to standardized procedures.
Additionally, Flora’s bill would remove any requirement that nurse anesthetists be supervised by a physician or dentist who requested anesthesia to be administered. That means a CRNA could be fully in charge of anesthesia for a patient’s surgery.
The bill would do away with industry assumptions that nurse anesthetists performing anesthesia services are supervised by a physician, dentist or other health care provider in the room. AB 876 also proposes that:
- Nurse anesthetists have authority to choose the modality of anesthesia and abort or change the modality during the surgery or care.
- In a hospital, outpatient center or dental office, nurse anesthetists could perform services beyond the preoperative setting, such as ordering, evaluating and interpreting diagnostic laboratory and radiological studies and issuing orders to nurses and other staff.
- Nurse anesthetists be allowed to provide sedation and pain management for palliative care.
Ordering and administering controlled substances and other drugs would not constitute a prescription.
The California Association of Nurse Anesthesiology, or CANA, has lobbied for giving more authority to CRNAs and donated $11,000 to Flora’s 2024 reelection campaign. Flora also received $11,000 from the California Society of Anesthesiologists.
Flora proposes a second bill, AB 1215, to expand hospital medical staff membership to include nurse anesthetists, nurse practitioners and nurse midwives.
Flora says bills ‘rebuild trust in our health care delivery system’
In a news release Friday, Flora said his proposed legislation was precipitated by California Department of Public Health surveys at hospitals in Stanislaus County in the past 18 months. Those surveys disagreed with the notion that CRNAs can practice independently.
“Regulatory confusions and misinterpretations have not only threatened the availability of essential anesthesia services in California, but also risked patient safety,” Flora said in the news release. “These two bills provide much-needed clarity to address workforce challenges, rebuild trust in our health care delivery system and ensure quality care without disruption.”
The CDPH survey at Stanislaus Surgical Hospital in February 2024 stated that unsupervised CRNAs placed patients in immediate jeopardy, and the agency suspended their work at the hospital. The CDPH did not lift the order until the short-stay hospital submitted a plan for using physician anesthesiologists. The CRNAs, who had the same status as anesthesiologists at the hospital, were laid off.
The state agency also temporarily barred nurse anesthetists from Doctors Medical Center in May 2024 because they had not been properly credentialed.
The CDPH survey, done on behalf of the federal Centers for Medicare and Medicare Services (CMS), criticized the work of CRNA staff at Stanislaus Surgical Hospital, including questionable decisions in prescribing drugs, sloppy paperwork, not getting patient consent for changing prescribed drugs and not communicating what drugs were given to patients.
The survey blasted Stanislaus Surgical Hospital for a disorganized medical staff. In-house doctors were not available for patients who suffered emergency complications after surgery or did not know how to treat anesthesia complications. Staff often called an ambulance to take those patients to another hospital, sometimes after a CRNA or physician assistant did not evaluate or provide medical care to the struggling patient.
The agency survey included a review of emergency patient transfers to other hospitals due to serious post-surgery complications in 2023. It attributed 10 of the emergency transfers to lack of supervision from physician anesthesiologists. Facing CMS requirements to correct myriad problems (not just anesthesia issues), Stanislaus Surgical closed in September.
CANA, the association for nurse anesthetists, has countered that the survey team was biased against CRNAs. “We’re grateful to Assemblymember Flora for his efforts to stand up for patients, improve health outcomes and maintain provider accountability,” said Emily Francke, a CRNA and CANA’s president, in the news release. “Together, we’re committed to protecting and — more importantly — increasing access to high-quality, safe and timely anesthesia care for Californians throughout the state.”
Bill would lower safety standards, anesthesia group says
Dr. Antonio Hernandez Conte, past president of California Society of Anesthesiologists, said the problems at Stanislaus Surgical Hospital are an example of independent CRNA practice. AB 876 will lower safety standards and remove any physician involvement from anesthesia care, he said.
“It certainly is out of line with the best practices nationally and has the potential to threaten the lives of California patients,” Conte said. “It does so by lowering safety standards and removing any and all physician involvement from anesthesia care.”
Conte noted that studies have shown CRNA independent practice in rural areas of the country does not result in a measurable improvement in patient access to care. Patients in rural areas, which may have higher rates of chronic disease, deserve to benefit from the 16,000 hours of education of a physician anesthesiologist, Conte said.
He said details in the proposed bill are a concern, such as allowing nurse anesthesia practices to bypass standardized procedures. “It removes the physician (anesthesiologist) from making the call for the kind of anesthesia indicated, bypasses their expertise and completely bypasses the safety test. It (bypasses) our system of checks and balances,” Conte said.
The CSA president said it remains to be seen how AB 876 would affect the collaborative teams at many hospitals, which consist of physician anesthesiologists supervising CRNAs.
Franke, representing CANA, said that many studies have shown health outcomes are similar whether a physician anesthesiologist or nurse anesthetists are in charge of care in states like California. By clarifying state statutes and allowing health care facilities to comprehensively assess anesthesia providers, Franke said, the two bills will prevent misinterpretations that can lead to unnecessary disruptions in care for patients.
Nurse anesthetists have almost three years of critical care experience before beginning an anesthesia program and undergo 2,600 hours of clinical training through the program, according to the American Association of Nurse Anesthesiology.
Doctors Medical Center and Emanuel hospital in Turlock have been required to adopt anesthesia models to settle issues with CDPH, according to CANA, which cited information from its members at those hospitals. The CRNAs are working under team models at the hospitals, with one physician anesthesiologist supervising three or four CRNAs during surgeries.
CDPH did not provide details on the ratio of physician anesthesiologists to CRNAs at DMC and Emanuel when asked last week. The team model also was imposed at a Southern California hospital, CANA says.
Collaboration teams including physician anesthesiologists and CRNAs are routinely in use at Kaiser Permanente hospitals, University of California medical centers and other facilities.
In September, the CDPH released an all-facilities letter reminding hospitals about CRNA scope-of-practice definitions. The agency letter said the use of CRNAs in acute care hospitals must be approved by administration and must be at the discretion of physicians. Nurse anesthetists may administer only anesthesia medications ordered by a physician and are not authorized to practice medicine, the agency said.
UPDATE: This story was updated to include more on the clinical experience and training of CRNAs. Nurse anesthetists have almost three years of critical care experience before beginning an anesthesia program and undergo 2,600 hours of clinical training through the program, according to the American Association of Nurse Anesthesiology. The story was also updated to report $11,000 in campaign donations of Assemblyman Heath Flora from the California Society of Anesthesiologists.
This story was originally published February 25, 2025 at 6:00 AM.
