Los Banos woman survived COVID-19 thanks to doctors she never met in person
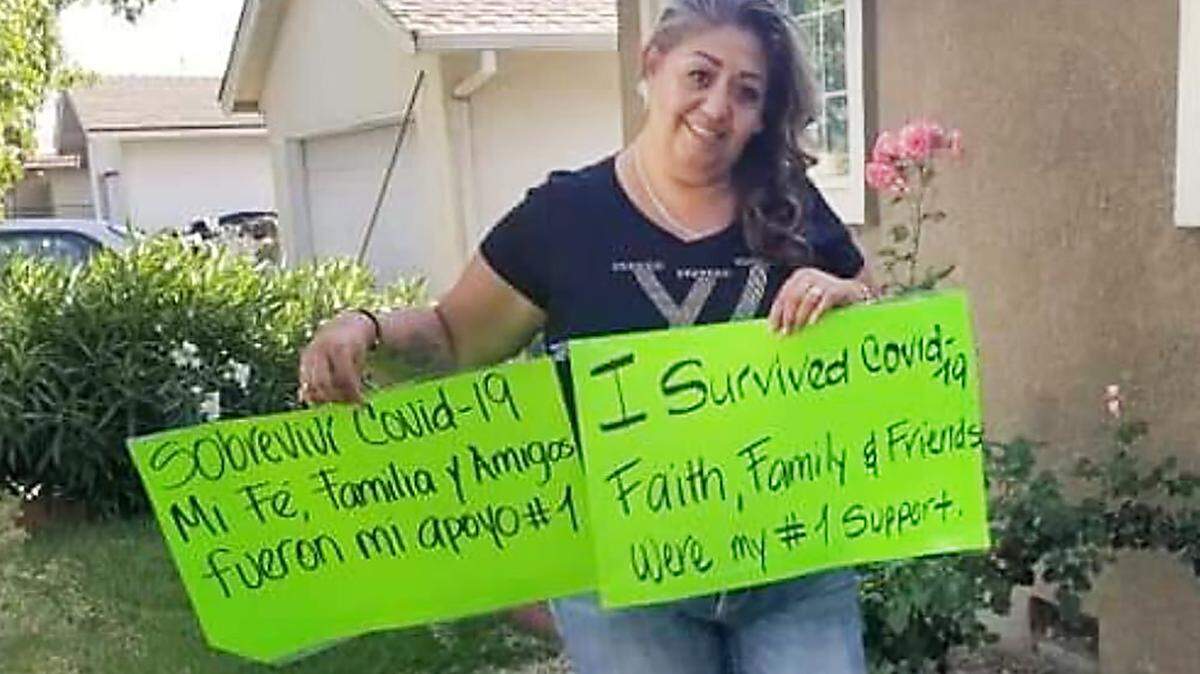
No one was more surprised than Rebeca Calderon herself when she was able to go home after surviving COVID-19 and a seven-day ICU stay at Memorial Hospital Los Banos. Last spring, she was their first COVID-19 patient.
The 48-year-old local resident was sure she was going to die when the doctors told her she needed to be on a breathing machine.
She lives alone, as her husband is in Mexico awaiting his immigration hearing. She has three adult sons who live in the area. One of them living in Modesto called 911 when he heard her breathing difficulties on the phone.
“I was really scared,” said Calderon. “I remember the doctor saying you’re positive and we have to give you the ventilator.” Her oxygen level was 50%, about half of what it should be.
She said, “I closed my eyes and said ‘God, help me.’ ”
She didn’t really understand what needing a ventilator meant or what telemedicine was, but ICU doctors in Sacramento, who never touched Calderon, helped save her life.
Telemedicine ICU is a system that connects a command center hub team of specially trained intensive care doctors, called intensivists, and nurses, with geographically distant ICU medical teams to assist with the care of critically ill patients using real-time audio, visuals and electronic medical information.
Sutter Health has one of the nation’s first telemedicine ICUs, called electronic-ICU or e-ICU, in the United States, and Memorial Hospital Los Banos was one of their first rural sites.
Memorial Hospital Los Banos is small, with only 30 licensed beds and a single, open-room ICU with four beds and no intensivists. Often their severely ill patients require transfer to larger hospitals, usually Memorial Medical Center in Modesto.
Last winter, Sutter Health optimized their almost 20-year-old e-ICU system, as much of the software and devices needed to be updated. They didn’t know how essential e-ICU would become in caring for COVID-19 patients.
“We went live with our reinvigorated e-ICU on January 29, right before COVID hit,” said Dr. Vanessa Walker, a pulmonary critical care physician and director of the e-ICU for the Valley area of Sutter Health.
Walker said Sutter Health’s e-ICU system has two central hubs, one in San Francisco covering the Bay Area and one in Sacramento, where she works covering the Valley area, which encompasses 10 hospitals. Five of those hospitals do not have intensivists.
Stationed in the central hub are four intensive care nurses and one intensivist at all times, each with a desk holding eight screens displaying remote patient data, including cardiac monitoring, lab results, vital signs and electronic medical records with essential information to manage a patient’s care. They can toggle into information on about 170 ICU patients in the Valley area.
At the remote ICU bedsides are pan-tilt zoom cameras that permit high resolution visualization of the patient, as well as iPads or computers for communications of the bedside medical team with the hub nurses and doctors.
Memorial Hospital in Los Banos has a hospital-based doctor and emergency room physician on duty 24/7. They can perform most procedures in collaboration with the e-ICU intensivist. The Los Banos staff also includes a surgeon who can be called in. The local physicians and nurses work closely with the e-ICU hub medical team.
“It feels like they’re right there,” Sheila Gonzales, ICU nurse at Los Banos, said of the e-ICU team.
Gonzalez said she had previous experience in another country caring for patients with Middle East Respiratory Syndrome, MERS, which was caused by a similar coronavirus, so she felt prepared for COVID-19 patients.
She said they couldn’t place COVID-19 patients in the open, one-room ICU. They had to arrange for private rooms nearby with proper ventilation to protect against the droplet spread of the coronavirus. They also had to adapt the e-ICU devices, including using iPads, to the new rooms.
e-ICU preserves ICU beds in Modesto
Memorial Medical Center in Modesto has 36 ICU beds, as well as a large group of intensivists, and it’s often the recipient of critically ill patients transferred from the smaller rural hospitals, including from Los Banos.
Over the past few weeks, with the surge of COVID-19 patients requiring the highest level of intensive care, Memorial Medical Center, as well as other ICUs in Modesto, have been operating near full, and at times beyond capacity.
“The remote e-ICU provides critical care 24/7,” said Dr. Ash Gokli chief medical officer of Sutter Health Valley Area, “By doing this we can keep patients locally and avoid transports, which improves patient safety.”
Walker said the e-ICU system avoiding patient transfers provides an extra buffer to help maintain resources and personnel in Modesto and the other larger hospitals.
Miriam Rivas, nurse manager at Los Banos, said they have taken care of about 10 COVID-19 patients and with the e-ICU support, they have been able to keep most of them in Los Banos. Two had to be transferred to Sacramento for highly specialized services.
“For those we had to transfer, the e-ICU helped us with the transfer,” said Rivas.
Not needing to transfer COVID-19 patients can be lifesaving.
“They’re very unstable, their oxygenation levels are terribly low,” said Walker, “...Putting them in an airplane or vehicle is putting their lives at risk.”
Walker also has a masters degree in clinical informatics, which she describes as “marrying technology with medicine.”
She said she sees telemedicine as the future of medicine, as it leverages technology to provide health care to everybody, regardless of where they are.
“If you choose to live in a rural community, it doesn’t mean your health should suffer because you don’t have access to the resources that you need,” said Walker.
The pandemic has increased the use of telemedicine, which previously had a tepid response by doctors and patients, with a common concern being the loss of the in-person connection.
For e-ICU care, the rise in popularity may fill in the gaps for intensive care services, which are in short supply nationwide, especially in rural communities. There aren’t enough intensivists or properly equipped ICUs in the U.S. to meet the growing demand with the aging population and the increased complexity of medical treatments.
Gonzales said the only hiccup she has had using e-ICU was a few times the WiFi was unstable, but those have been brief.
“It’s great knowing that they’re there and they listen to the bedside nurses,” said Gonzales.
Nurse to e-ICU nurse
“You don’t know what you don’t know,” said Jacob Aldridge, assistant nurse manager in Los Banos. “(The e-ICU) provides a wealth of knowledge and ideas...for interventions you might not have thought of or didn’t know.”
The e-ICU nurses offer support and education for the remote ICU nurses. For example, the e-ICU nurses taught the Los Banos nurses how to do prone positioning for COVID-19 patients, including those on ventilators. Placing the patients on their stomach has emerged as a life-saving maneuver for COVID-19 patients.
Nursing supervisor Rivas said Calderon was so sick that the medical team was afraid she wouldn’t survive.
Calderon said when she was waking up from the medically induced coma she could hear the nurse calling her name but couldn’t respond.
“I can see the tears in the nurse’s eyes because she was so happy to see me wake up,” said Calderon, “She said she had been praying for me every day.”
When she was discharged, the medical team had a parade for her.
“When she left the hospital, she was crying, the nurses were crying, it was very emotional,” said Rivas.
Calderon said leaving the hospital was very emotional for her, too. At first, she couldn’t talk about the experience without crying. She said her recovery has been slow and that almost five months later, she is still not herself.
“This COVID thing has changed my life,” said Calderon.
She said she doesn’t have the stamina to return to her job as a cannery supervisor, she still has some coughing, can’t walk long distances because she gets short of breath and her “brain just isn’t the same.”
Calderon said she doesn’t have the words to express her gratitude for the care and compassion that she received from the doctors and nurses.
“I’m alive for a purpose,” said Calderon, “ I know I’m going to be OK.”
This story was produced with financial support from The Stanislaus County Office of Education and the Stanislaus Community Foundation, along with the GroundTruth Project’s Report for America initiative. The Modesto Bee maintains full editorial control of this work.
This story was originally published September 3, 2020 at 4:00 AM.
